GET RELIEF, WITHOUT THE ADDICTION.

MICHIGAN'S OPIOID CRISIS
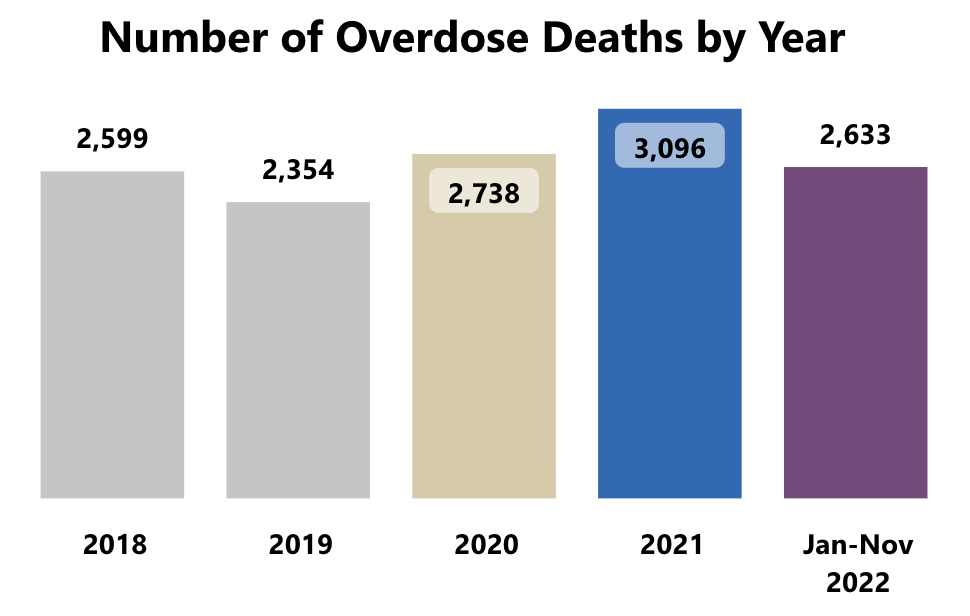
3,096
Overdose deaths (2021)
2,633
Opioid deaths
(Jan – Nov 2022)
428
For every 100,000
hospital visits, 428 are opioid related
(January – December 2021)
WHAT ARE OPIOIDS?
Opioids are a class of prescription pain reliever that interacts with opioid receptors on nerve cells in the brain and body. In addition to pain relief, opioids can produce euphoria (a feeling of intense happiness) – this is why they are often misused. Misuse (using in a different way or a larger quantity than prescribed or taken without a prescription) can lead to addiction, overdose, and death. In addition, misuse of prescription opioids often leads to use of illegal street drugs, once the supply of prescription drugs is ended.
WHAT OPIOIDS ARE FOR:
Opioids are pain-relieving drugs that are meant to help control severe pain such as what you experience after surgery.
CAN OPIOIDS TREAT BACK PAIN?
In the 1990s and early 2000s, pharmaceutical companies (incorrectly) marketed opioids to prescribing physicians as nonaddictive and highly effective for all pain, including lower back pain. Even now, after all we know about the dangers of opioids, some physicians still prescribe them for neck, back and muscle pain, often with poor results, as many patients continue to report chronic pain and a decreased quality of life.
TREAT PAIN WITHOUT OPIOIDS
Opioids only mask symptoms, they do nothing to alleviate the problem causing the pain in the first place. Many leading health care agencies – including the Centers for Disease Control and Prevention, the U.S Food & Drug Administration, the U.S. Department of Health and Human Services, the National Academy of Medicine, The Joint Commission on the Accreditation of Healthcare, and the Veterans Affairs Health System – recommend conservative, drug- and surgery-free care like chiropractic as a first line of defense for patients with non-cancer-related pain. The fact is this: Opioids must be a last resort for the treatment of neck, back, and muscle pain.
Michigan Opioid Data:
An opioid can be a prescription drug, often referred to as painkillers, or an illicit substance, such as heroin. Find out more about the opioid epidemic in Michigan.
Since 2000, opioid overdose deaths have grown tenfold in Michigan. This epidemic impacts thousands of Michiganders and their families, friends, and communities. It’s one of the greatest public health crises of our lifetimes, and we must respond urgently.
Image Source: Michigan Overdose Data to Action
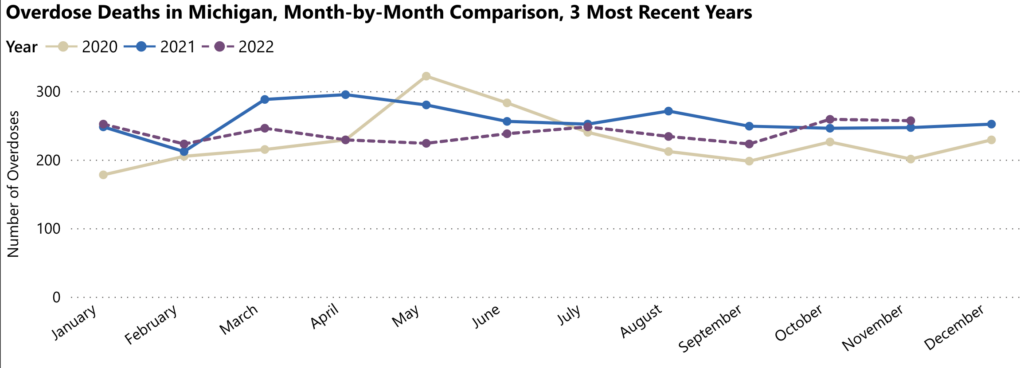
Image Source: Michigan Overdose Data to Action
Michigan Chiropractors Relieve Pain Using a Non-Drug, Non-Surgical Approach
The public, the Governor and health officials working to continue Michigan’s declines in drug overdose rates.
NALOXONE
In the event of an opioid overdose, there is a drug that can be used that can reverse the effects of the opioid. Naloxone (commonly known by the brand names Narcan and Evzio) is a life-saving medication used to reverse the effect of an opioid overdose. Naloxone is not addictive. Payment for the medication Naloxone is covered by Medicaid and many other insurances. Many non-profit organizations also distribute Naloxone.
Use the map to the right to find an approved pharmacy near you.
Why Carry Naloxone?
Naloxone saves lives
Nearly 50,000 people died from an opioid-involved overdose in 2019. One study found that bystanders were present in more than one in three overdoses involving opioids. With the right tools, bystanders can act to prevent overdose deaths. Anyone can carry naloxone, give it to someone experiencing an overdose, and potentially save a life.
Who Should Carry Naloxone?
If you or someone you know is at increased risk for opioid overdose, especially those struggling with opioid use disorder (OUD), you should carry naloxone and keep it at home. People who are taking high-dose opioid medications (greater or equal to 50 morphine milligram equivalents per day) prescribed by a doctor, people who use opioids and benzodiazepines together, and people who use illicit opioids like heroin should all carry naloxone. Because you can’t use naloxone on yourself, let others know you have it in case you experience an opioid overdose.
Carrying naloxone is no different than carrying an epinephrine auto-injector (commonly known by the brand name EpiPen) for someone with allergies. It simply provides an extra layer of protection for those at a higher risk for overdose.
Source: CDC
Get Help:
If you or someone you know needs help with opioid use disorder, call the SAMSHA National Hotline, a 24-hour, 365-day-a-year, treatment referral hotline.
Signs of Overdose
Recognizing the signs of opioid overdose can save a life. Here are some things to look for:
- Small, constricted “pinpoint pupils”
- Falling asleep or losing consciousness
- Slow, weak, or no breathing
- Choking or gurgling sounds
- Limp body
- Cold and/or clammy skin
- Discolored skin (especially in lips and nails)
What to do if You Think Someone is Overdosing
It may be hard to tell whether a person is high or experiencing an overdose. If you aren’t sure, treat it like an overdose—you could save a life.
1
Call 911 Immediately.*
2
Administer naloxone, if available.
3
Try to keep the person awake
and breathing.
4
Lay the person on their side to
prevent choking.
5
Stay with the person until emergency assistance arrives.
*Michigan’s Good Samaritan law prevents drug possession charges against those that seek medical assistance for an overdose in certain circumstances.
Source: CDC
Chiropractic Care is Endorsed By: